Why Personalised Medicine Matters
Would a teenage boy buy the same clothes as his grandmother? Probably not. But when they get sick, they’re likely to receive the same medical treatment, despite their many differences. And so will everyone else.
That’s because even the world’s best scientists and doctors don’t fully understand yet how different people develop disease and respond to treatments.
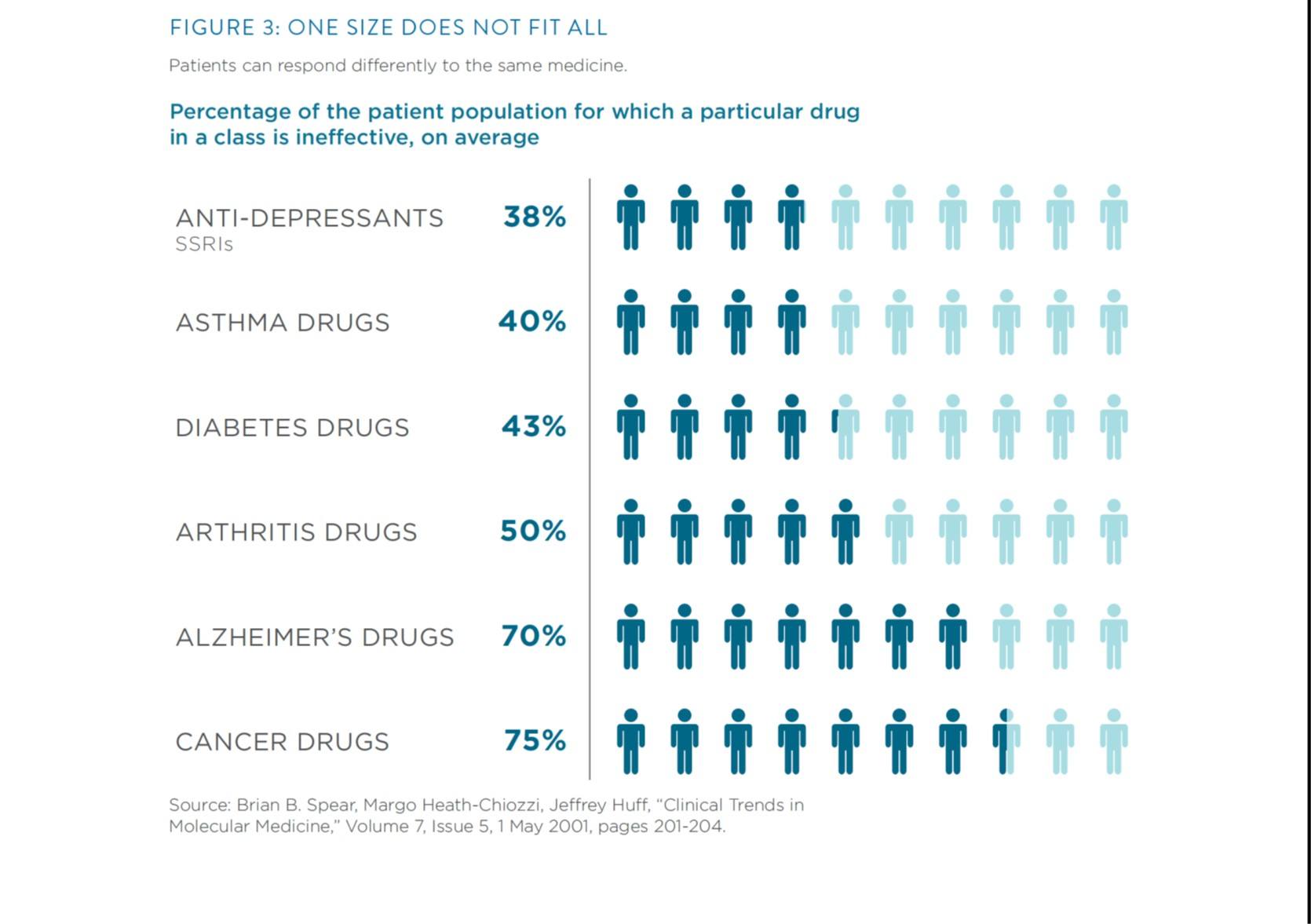
The result is a “one-size-fits-all” approach to medicine that is based on broad population averages. This traditional practice often misses its mark because each person’s genetic makeup is different from everyone else’s, often in very important ways that affect health.
The advent of personalised medicine is moving us closer to more precise, predictable and powerful health care that is customized for the individual patient. Our growing understanding of genetics and genomics – and how they drive health, disease and drug responses in each person – is enabling doctors to provide better disease prevention, more accurate diagnoses, safer drug prescriptions and more effective treatments for the many diseases and conditions that diminish our health.
Tailoring health care to each person’s unique genetic makeup – that’s the promising idea behind personalised medicine, also variously known as individualized medicine, precision medicine or genomic medicine.
11 Ways Personalised Medicine is Helping People
- Shifting the emphasis in medicine from reaction to prevention
- Predicting susceptibility to disease
- Improving disease detection
- Pre-empting disease progression
- Revealing additional or alternative uses for medicines and drug candidates
- Customising disease-prevention strategies
- Increasing patient adherence to treatment
- Prescribing more effective drugs
- Avoiding prescribing drugs with predictable side effects
- Reducing the time, cost, and failure rate of pharmaceutical clinical trials
- Eliminating trial-and-error inefficiencies that inflate health care costs and undermine patient care






Social Links